Impact Factor
Theranostics 2022; 12(14):6179-6188. doi:10.7150/thno.76571 This issue Cite
Research Paper
What a difference a methylene makes: replacing Glu with Asp or Aad in the Lys-urea-Glu pharmacophore of PSMA-targeting radioligands to reduce kidney and salivary gland uptake
1. Department of Molecular Oncology, BC Cancer, Vancouver, BC V5Z1L3, Canada.
2. Department of Functional Imaging, BC Cancer, Vancouver, BC V5Z4E6, Canada.
3. Department of Radiology, University of British Columbia, Vancouver, BC V5Z1M9, Canada.
Abstract
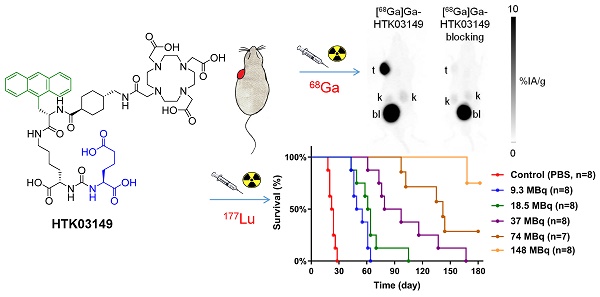
The aim of this study was to investigate the effect of replacing Glu in the Lys-urea-Glu PSMA-targeting pharmacophore of [68Ga]Ga-HTK03041 with a close analog on the uptake of kidneys, salivary glands and PSMA-expressing tumor xenografts.
Methods: HTK03161, HTK03149 and HTK03189A/B were obtained by replacing Glu in HTK03041 with Asp, Aad (L-2-aminoadipic acid) and Api (2-aminopimelic acid), respectively. PSMA binding affinities were measured by competition binding assays. PET imaging and biodistribution studies of 68Ga-labeled ligands were performed in LNCaP tumor-bearing mice. The best candidate HTK03149 was selected and radiolabeled with 177Lu, and SPECT imaging and biodistribution studies were performed in LNCaP tumor-bearing mice. Radiation dosimetry calculation was conducted using the OLINDA software. Radioligand therapy study was performed in LNCaP tumor-bearing mice treated with [177Lu]Lu-HTK03149 (9.3-148 MBq), [177Lu]Lu-PSMA-617 (37 MBq) or natLu-HTK03149 (500 pmol).
Results: PSMA binding affinities (Ki) of Ga-HTK03161, Ga-HTK03149, Ga-HTK03189A and Lu-HTK03149 were 3.88±0.66, 6.99±0.80, 550±35.7 and 1.57±0.42 nM, respectively. PET imaging showed that all 68Ga-labeled HTK03161, HTK03149 and HTK03189A/B were excreted mainly via the renal pathway and had minimal uptake in all organs/tissues including kidneys and salivary glands. Tumor xenografts were clearly visualized in PET images of [68Ga]Ga-HTK03161 and [68Ga]Ga-HTK03149 but were barely visualized using [68Ga]Ga-HTK03189A/B. Tumor uptake values for [68Ga]Ga-HTK03161, [68Ga]Ga-HTK03149, [68Ga]Ga-HTK0189A and [68Ga]Ga-HTK03189B were 12.7±1.91, 19.1±6.37, 2.10±0.28 and 0.67±0.15 %IA/g, respectively at 1h post-injection, and their average kidney and salivary gland uptake values were 2.13-4.41 and 0.20-0.23 %IA/g, respectively. Longitudinal SPECT imaging studies showed that [177Lu]Lu-HTK03149 was excreted mainly through the renal pathway with high uptake in LNCaP tumors and minimal uptake in all normal organs/tissues. The tumor uptake of [177Lu]Lu-HTK03149 peaked at 4h post-injection (20.9±2.99 %IA/g) and the uptake was sustained over time. Compared to [177Lu]Lu-PSMA-617, [177Lu]Lu-HTK03149 had 145% increase in tumor absorbed dose but 70% less in kidney absorbed dose, leading to an 7.1-fold increase in tumor-to-kidney absorbed dose ratio. Radioligand therapy studies showed that only half of the [177Lu]Lu-PSMA-617 injected dosage was needed for [177Lu]Lu-HTK03149 to achieve the same median survival.
Conclusion: Replacing Glu in the PSMA-targeting Lys-urea-Glu pharmacophore of [68Ga]Ga-HTK03041 with Asp and Aad generates [68Ga]Ga-HTK03161 and [68Ga]Ga-HTK03149, respectively, and the new derivatives retain high uptake in LNCaP tumors and have minimal uptake in normal organs/tissues including kidneys and salivary glands. [177Lu]Lu-HTK03149 also retain high uptake in LNCaP tumors and has minimal uptake in normal organs/tissues, and is, therefore, promising for clinical translation to treat prostate cancer.
Keywords: Prostate-specific membrane antigen, Salivary gland, Off-target uptake, Targeted radioligand therapy, Tumor-to-kidney absorbed dose ratio
 Global reach, higher impact
Global reach, higher impact