13.3
Impact Factor
Theranostics 2022; 12(7):3024-3044. doi:10.7150/thno.57218 This issue Cite
Research Paper
Critical role of FPR1 in splenocyte migration into brain to worsen inflammation and ischemic brain injury in mice
1. Department of Anesthesiology, University of Virginia, Charlottesville, Virginia 22908, USA.
2. Department of Radiology and Biomedical Imaging, University of Virginia, Charlottesville, VA, 22908, USA.
3. Department of Microbiology, Immunology, and Cancer Biology, University of Virginia, Charlottesville, VA, USA.
Abstract
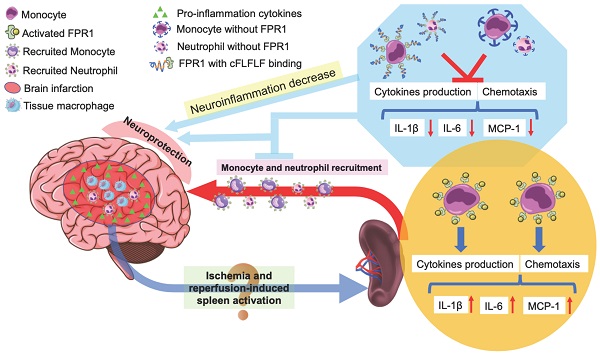
Background: Splenocyte contribution to ischemic brain injury has been suggested. It is not known whether this effect is due to systemic action or direct influence in ischemic brain tissues. It is also not known how splenocytes migrate into the brain and worsen neurological outcome after brain ischemia. We determined the role of formyl peptide receptor 1 (FPR1), a receptor expressed in monocytes, in the migration of splenocytes into ischemic brain tissues and the contribution of these splenocytes to ischemic brain injury.
Methods: Mice with or without fpr1 knockout were subjected to transient focal brain ischemia. The migration of splenocytes was assessed under in vivo and in vitro conditions.
Results: cFLFLF, a FPR1 antagonist, inhibited splenocyte migration into the brain and neuroinflammation after ischemic stroke. cFLFLF improved neurological outcome assessed 24 hours or 28 days after stroke. cFLFLF did not alter blood-brain barrier permeability in the ischemic brain. fpr1-/- mice had an attenuated peripheral monocyte and neutrophil infiltration into the brain, a reduced proinflammatory cytokine level and an improved neurological outcome compared with wild-type mice after brain ischemia. cFLFLF did not affect the proinflammatory cytokine levels in the spleen and brain of fpr1-/- mice after ischemic stroke.
Conclusions: These results suggest that FPR1 facilitates splenocyte migration into the brain and proinflammatory cytokine production to worsen neurological outcome after brain ischemia, indicating a direct effect of splenocytes on ischemic brain tissues. Our results support the notion that cFLFLF via blocking FPR1 signaling inhibits those pathological processes and is a potential agent for neuroprotection.
Keywords: Brain imaging, brain ischemia, formyl peptide receptor 1, splenocyte migration, neuroinflammation, neuroprotection
 Global reach, higher impact
Global reach, higher impact