Impact Factor
Theranostics 2020; 10(12):5384-5397. doi:10.7150/thno.41616 This issue Cite
Research Paper
Targeted sequencing reveals the mutational landscape responsible for sorafenib therapy in advanced hepatocellular carcinoma
1. Cancer Center, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430022, China.
2. The International Cooperation Laboratory on Signal Transduction, Eastern Hepatobiliary Surgery Hospital, Second Military Medical University, Shanghai 200438, China.
3. Department of special treatment and liver transplantation, Eastern Hepatobiliary Surgery Hospital, Second Military Medical University, Changhai Road 225, Shanghai 200438, China
4. MOE Key Laboratory for Bioinformatics, BNRIST Bioinformatics Division, Department of Automation, Tsinghua University, Beijing 100084, China
5. Department of Pathology, Eastern Hepatobiliary Surgery Hospital, Second Military Medical University, Changhai Road 225, Shanghai, Shanghai 200438, China
6. Department of Clinical Pharmacology, Xiangya Hospital, Central South University, Changsha, Hunan, China. 2Institute of Clinical Pharmacology, Central South University, Changsha, Hunan 410013, China.
7. Department of Liver Surgery, Renji Hospital, School of Medicine, Shanghai Jiao Tong University, Shanghai, 200127, China.
8. Department of Biliary Surgery I, Eastern Hepatobiliary Surgery Hospital, Second Military Medical University, Changhai Road 225, Shanghai 200438, China
9. The United Innovation of Mengchao Hepatobiliary Technology Key Laboratory of Fujian Province, Mengchao Hepatobiliary Hospital of Fujian Medical University, Fuzhou 350025, China
10. Fudan University Shanghai Cancer Center; Department of Oncology, Shanghai Medical College, Fudan University, Shanghai 200032, China
11. Ministry of Education (MOE) Key Laboratory on signaling Regulation and Targeting Therapy of Liver Cancer, Shanghai 200438, China
12. Shanghai Key Laboratory of Hepato-biliary Tumor Biology, Shanghai 200438, China
# These authors contributed equally to this work.
Abstract
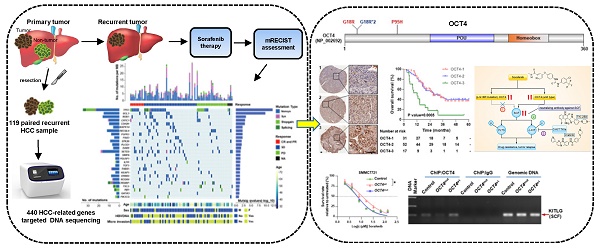
Rationale: The existence of primary and acquired drug resistance is the main obstacle for the effect of multi-kinase inhibitor sorafenib and regorafenib in advanced hepatocellular carcinoma (HCC). However, plenty of patients did not significantly benefit from sorafenib treatment and little is known about the mechanism of drug resistance.
Methods: Laser capture microdissection was used to acquire matched normal liver and tumor tissues on formalin-fixed paraffin-embedded specimens collected before sorafenib therapy from the first surgery of 119 HCC patients. Ultra-deep sequencing (~1000×) targeting whole exons of 440 genes in microdissected specimens and siRNA screen in 7 cell lines were performed to find mutations associated with differential responses to sorafenib. Patient-derived xenograft models were employed to determine the role of TP53 in response to sorafenib. Lentiviruses harboring wild-type and c.G52C-mutant OCT4 were applied to explore the function of OCT4 in resistance to sorafenib. ChIP-PCR assay for analysis of OCT4 transcriptional activity was performed to explore the affinity with the KITLG promoter. Statistical analyses were used to associate levels of p53 and OCT4 with tumor features and patient outcomes.
Results: Total 1,050 somatic mutations and 26 significant driver genes were identified. SiRNA screening in 7 HCC cell lines was further performed to identify mutations associated with differential responses to sorafenib. A recurrent nonsynonymous mutation c.G52C in OCT4 (OCT4mut) was strongly associated with good response to sorafenib, whereas the stop-gain mutation in TP53 showed the opposite outcome both in vitro and in vivo. OCT4wt-induced stem cell factor (encoded by KITLG gene, SCF) expression and cross-activation of c-KIT/FLT3-BRAF signals were identified indispensably for sorafenib resistance, which could be reversed by the combination of c-KIT tyrosine kinase inhibitors or neutralizing antibody against SCF. Mechanistically, an OCT4 binding site in upstream of KITLG promoter was identified with a higher affinity to wildtype of OCT4 rather than G52C-mutant form, which is indispensable for OCT4-induced expression of KITLG and sorafenib resistance.
Conclusion: Our study reported a novel somatic mutation in OCT4 (c.G52C) responsible for the sorafenib effect, and also shed new light on the treatment of HCC through the combination of specific tyrosine kinase inhibitors according to individual genetic patterns.
Keywords: Mutational Landscape, Sorafenib Resistance, TP53, OCT4, Hepatocellular Carcinoma.
 Global reach, higher impact
Global reach, higher impact