13.3
Impact Factor
Theranostics 2021; 11(2):768-788. doi:10.7150/thno.50540 This issue Cite
Research Paper
Implantation of regenerative complexes in traumatic brain injury canine models enhances the reconstruction of neural networks and motor function recovery
1. Tianjin Key Laboratory of Neurotrauma Repair, Institute of Traumatic Brain Injury and Neuroscience, Center for Neurology and Neurosurgery of Characteristic Medical Center of Chinese People's Armed Police Force (PAP), Chenglin Road No.220, Tianjin 300162, China.
2. Postgraduate school, Medical school of Chinese People's Liberation Army (PLA), General Hospital of PLA, Fuxing Road No. 28, Beijing 100853, China.
3. Department of Neurosurgery, West China Hospital, West China Medical School, Sichuan University, Chengdu, Sichuan 610041, China
4. Department of Neurology, the Armed Police Corps Hospital of Zhejiang Province, Hangzhou 310000, China.
5. Tianjin Key Laboratory of Oral and Maxillofacial Function Reconstruction, Tianjin Stomatological Hospital, Tianjin 300041, China.
6. SUSTech-UTokyo Joint Research Center on Super Smart City, Southern University of Science and Technology, Center for Spatial Information Science, The University of Tokyo, Tokyo 277-8568, Japan.
7. Department of pathology, Characteristic Medical Center of Chinese People's Armed Police Force (PAP), Chenglin Road No.220, Tianjin 300162, China.
8. Department of Neurosurgery of Tianjin Fourth Central Hospital, Zhongshan Road No.1, Tianjin 300143, China.
*These authors contribute equally to this work.
Abstract
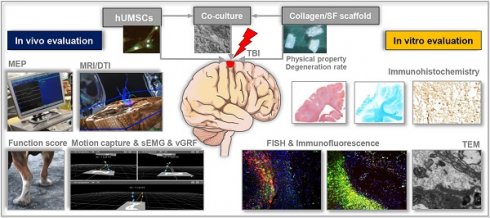
Rationale: The combination of medical and tissue engineering in neural regeneration studies is a promising field. Collagen, silk fibroin and seed cells are suitable options and have been widely used in the repair of spinal cord injury. In this study, we aimed to determine whether the implantation of a complex fabricated with collagen/silk fibroin (SF) and the human umbilical cord mesenchymal stem cells (hUCMSCs) can promote cerebral cortex repair and motor functional recovery in a canine model of traumatic brain injury (TBI).
Methods: A porous scaffold was fabricated with cross-linked collagen and SF. Its physical properties and degeneration rate were measured. The scaffolds were co-cultured with hUCMSCs after which an implantable complex was formed. After complex implantation to a canine model of TBI, the motor evoked potential (MEP) and magnetic resonance imaging (MRI) were used to evaluate the integrity of the cerebral cortex. The neurologic score, motion capture, surface electromyography (sEMG), and vertical ground reaction force (vGRF) were measured in the analysis of motor functions. In vitro analysis of inflammation levels was performed by Elisa while immunohistochemistry was used in track the fate of hUCMSCs. In situ hybridization, transmission electron microscope, and immunofluorescence were used to assess neural and vascular regeneration.
Results: Favorable physical properties, suitable degradation rate, and biocompatibility were observed in the collagen/SF scaffolds. The group with complex implantation exhibited the best cerebral cortex integrity and motor functions. The implantation also led to the regeneration of more blood vessels and nerve fibers, less glial fibers, and inflammatory factors.
Conclusion: Implantation of this complex enhanced therapy in traumatic brain injury (TBI) through structural repair and functional recovery. These effects exhibit the translational prospects for the clinical application of this complex.
Keywords: Hemiplegic limb, Collagen, Silk fibroin, Mesenchymal stem cell, Traumatic brain injury
 Global reach, higher impact
Global reach, higher impact