13.3
Impact Factor
Theranostics 2019; 9(24):7403-7416. doi:10.7150/thno.32637 This issue Cite
Research Paper
Incorporation of small extracellular vesicles in sodium alginate hydrogel as a novel therapeutic strategy for myocardial infarction
1. Department of Cardiology of The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, PR China;
2. Cardiovascular Key Laboratory of Zhejiang Province, Hangzhou, PR China;
3. Nanjing Medical University, Nanjing, PR China;
4. Institute of Translational Medicine, Zhejiang University, Hangzhou, PR China;
5. State Key Laboratory of Silicon Materials, School of Materials Science and Engineering, Zhejiang University, Hangzhou, Zhejiang 310027, PR China;
6. Center for Biomaterials and Biopathways, Department of ChemistryState Key Laboratory of Silicon Materials, School of Materials Science and Engineering, Zhejiang University, Hangzhou, Zhejiang 310027, PR China;
7. Department of Cardiology, Affiliated Hangzhou First People's Hospital, Zhejiang University School, Hangzhou, PR China.
*These authors contributed equally to this article.
Abstract
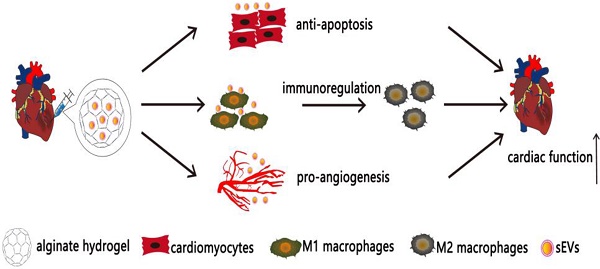
Bone marrow mesenchymal stem cell (MSC)-derived small extracellular vesicles (sEVs) have been widely used for treating myocardial infarction (MI). However, low retention and short-lived therapeutic effects are still significant challenges. This study aimed to determine whether incorporation of MSC-derived sEVs in alginate hydrogel increases their retention in the heart thereby improving therapeutic effects.
Methods: The optimal sodium alginate hydrogel incorporating sEVs system was determined by its release ability of sEVs and rheology of hydrogel. Ex vivo fluorescence imaging was utilized to evaluate the retention of sEVs in the heart. Immunoregulation and effects of sEVs on angiogenesis were analyzed by immunofluorescence staining. Echocardiography and Masson's trichrome staining were used to estimate cardiac function and infarct size.
Results: The delivery of sEVs incorporated in alginate hydrogel (sEVs-Gel) enhanced their retention in the heart. Compared with sEVs only treatment (sEVs), sEVs-Gel treatment significantly decreased cardiac cell apoptosis and promoted the polarization of macrophages at day 3 after MI. sEVs-Gel treatment also increased scar thickness and angiogenesis at four weeks post-infarction. Measurement of cardiac function and infarct size were significantly better in the sEVs-Gel group than in the group treated with sEVs only.
Conclusion: Delivery of sEVs incorporated in alginate hydrogel provides a novel approach of cell-free therapy and optimizes the therapeutic effect of sEVs for MI.
Keywords: sEVs, alginate, hydrogel, stem cells, myocardial infarction.
 Global reach, higher impact
Global reach, higher impact