Impact Factor
Theranostics 2014; 4(7):736-744. doi:10.7150/thno.8725 This issue Cite
Research Paper
The Prognostic Value of 18F-FDG PET/CT for Hepatocellular Carcinoma Treated with Transarterial Chemoembolization (TACE)
1. Department of Nuclear Medicine, Xijing Hospital, Fourth Military Medical University, Xi'an, China;
2. Department of Liver Disease and Digestive Interventional Radiology, Xijing Hospital of Digestive Diseases, Xijing Hospital, Fourth Military Medical University, Xi'an, China;
3. State Key laboratory of Cancer Biology and Xijing Hospital of Digestive Diseases, Xijing Hospital, Fourth Military Medical University, Xi'an, China.
*These authors contributed equally to this work.
Received 2014-1-30; Accepted 2014-3-24; Published 2014-5-1
Abstract
18F-Fluoro-deoxyglucose (FDG) PET/CT can be used to monitor the biological behavior of hepatocellular carcinoma (HCC). Baseline PET/CT has prognostic value in HCC patients, but there is litter knowledge of the PET/CT changes after treatment. We evaluated 27 HCC patients treated with transarterial chemoembolization (TACE) from June 2011 to July 2012, and we investigated the prognostic value of PET/CT. Patients were followed up with regular clinical and laboratory examinations and contrast-enhanced spiral computed tomography (CT). Furthermore, PET/CT assessments were collected and analyzed before (range 1~15 d) and after the first month of TACE (range, 27~45d). We tested the prognostic value of the tumor standardized uptake value (TSUV) and normal liver SUV(LSUV) according to the VOI (volume of interest). The SUVs were used to assess the relationship between the treatment response and survival. To assess their prognostic value, we evaluated the areas under the receiver operating characteristic (ROC) curves of different SUVs for predicting survival. Finally, the median overall survival (OS) and time to progression (TTP) for 27 patients were 15.4 months (95%CI, 3.3-27.5 months) and 11.4 months (95%CI, 6.7-16.1 months), respectively. The ΔTSUVmax%, based on the VOI, had the highest discriminative prognostic value and the cutoff PET/CT response was 0.1 with a sensitivity of 100% and a specificity of 95.2%. The OS was significantly better in the PET/CT response group than in the PET/CT non-response group (p=0.025). In conclusion, an early interim PET/CT after TACE may have prognostic value for HCC patients treated with TACE, and the ΔTSUVmax% may help in determining the HCCs viability in patients with high baseline and follow-up18F-FDG uptake.
Keywords: hepatocellular carcinoma, transarterial chemoembolization (TACE), positron-emission tomography (PET), computed tomography (CT).
Introduction
Transarterial chemoembolization (TACE) works by concentrating chemotherapeutic agents at the tumor site while blocking the tumor's primary feeding artery [1,2]. TACE also acts as a first-line, non-curative therapy for unresectable hepatocellular carcinoma (HCC), which has been confirmed by two randomized controlled trials and a meta-analysis [3-5]. Nonetheless, only 15-55% patients achieve a partial response after TACE therapy [6,7]. Therefore, assessing an accurate therapy response and prognosis is important for guiding further treatment. The European Association for the Study of the Liver (EASL) criteria and the modified Response Evaluation Criteria in Solid Tumors (mRECIST) have been widely used for TACE in the clinic [6]. However, the techniques for evaluating the morphology and the criteria based on contrast-enhanced computer tomography (CT) or magnetic resonance imaging (MRI) might not be in agreement with the actual biological assessment [6,8].
Positron emission tomography (PET) with 18F-2-fluoro-2-deoxyglucose (18F-FDG) has emerged in recent years and is widely used for baseline staging and monitoring the treatment response in various cancers. 18F-FDG PET/CT, which detects the glucose metabolic activity of tumors, provides useful information that cannot be obtained from other conventional imaging techniques, and 18F-FDG PET/CT allows for whole body surveillance [9,10]. Many studies have shown that 18F-FDG PET/CT is useful for tumor characterization, prognosis prediction, and assessment of the therapeutic response [11-13]. Based on their gene expression profiles, HCCs with high 18F-FDG uptake are reported to be more aggressive than HCCs with low 18F-FDG uptake [14]. Moreover, baseline PET/CT has great prognostic value for HCC patients who are treated with chemotherapy, radiotherapy, resection, TACE and Sorafenib [9,15-18]. However, previous studies have only focused on the prognostic value of the tumor baseline standard uptake value (SUV), and they did not assess the changes in the 18F-FDG-PET/CT response parameters with treatment. Evaluating the changes may provide a more accurate and objective evaluation of the tumors. Furthermore, a recent study from our team confirmed that an effective imaging evaluation time point for HCC patients after combination therapy with Sorafenib and transarterial chemoembolization is the third month, which is when the overall survival and therapy response have the closest relationship [19]. Thus, the response evaluation changes during therapy could provide much more information than a single baseline assessment.
Therefore, the aim of this study was to investigate the prognostic value of the 18F-FDG PET/CT response changes after TACE therapy in intermediate hepatocellular carcinoma patients.
Patients and Methods
From June 2011 to July 2012, a total of 35 intermediate HCC patients were treated with TACE and underwent a baseline FDG PET/CT scan. Eight patients did not undergo a PET/CT scan after the therapy; thus, a total of 27 patients were included in this study. All procedures were in accordance with the ethics committee of Xijing Hospital and with the Helsinki Declaration of 1975 (revised in 2008). Additional informed consent was obtained from all patients, and the patient demographics are included in this article. The inclusion criteria were the following: 1) age ≥18 years old, 2) confirmed diagnosis of HCC based on the American Association for the Study of Liver Disease (AASLD) criteria, 3) stage B HCC according to Barcelona Clinic Liver Cancer (BCLC), 4) preserved liver function with Child-Pugh Class A or B (≤7 score), 5) an Eastern Cooperative Oncology Group (ECOG) performance status of 0 or 1, and 6) no previous treatment. The exclusion criteria were the following: 1) diffuse HCC lesions; 2) heart, respiratory or renal dysfunction/failure; and 3) concurrent malignancy.
Treatments
Patients were treated with conventional TACE, which included the following procedures: 1) confirm the tumor feeding artery with abdominal angiography, 2) insert a catheter into the HCC feeding artery as close to the lesion as possible, and 3) infect the emulsion of 30-50 mg pirarubicin with 10-20 mg lipiodol and then inject the Gelatin foam or PVA embolization particles until the tumor feeding vessels are completely obstructed. The TACE procedure was repeated in lesions with incomplete tumor necrosis or regrowth or new hepatic lesions. A total of 10 patients repeated TACE therapy as recommended after undergoing a medical evaluation, which was based on their physical status; the second TACE therapy sessions were performed after the second PET/CT scans.
Follow-up
The patients were followed up with regular clinical examinations including blood tests and contrast-enhanced spiral computed tomography (CT) at one month (baseline, range 30~39 d) after the first TACE and every two months thereafter. Moreover, 18F-Fluoro-deoxyglucose (FDG) PET/CT assessments were performed before the first TACE (baseline or PET/CT1, range 1~15 d) and one month after TACE therapy (PET/CT2, range 27~45 d). The overall survival (OS) was measured from the beginning of the first TACE therapy to the date of death or the last follow-up. The time to progression (TTP) was defined as the time from the first TACE to radiological disease progression according to the modified Response Evaluation Criteria in Solid Tumors (mRECIST), which was based on the ratio change of the longest diameter of the enhancing lesion according to contrast-enhanced CT. Complete response (CR) was defined as a 100% decrease in the lesion, partial response (PR) was defined as at least a 30% decrease, progressive disease (PD) was defined as at least a 20% increase, and other findings were defined as stable disease (SD). Patients with CR or PR were considered responders. Patients with SD or PD were considered non-responders.
PET imaging acquisition and analysis
A whole body PET/CT scanner, Biograph TruePoint 40 PET/CT (Siemens Medical Systems, USA), was used to image all patients. Before the test, patients fasted for ≥6 hours, and their blood glucose levels were ≤140 mg/dl. Approximately 5.5 MBq/kg of body weight of 18F-FDG (275~528 MBq, 7.43 mCi~14.27 mCi) was administered intravenously and then all patients rested for 45 min. The 18F-FDG PET/CT scan was performed from the skull base to the proximal thigh. Images were reconstructed onto a square matrix, corrected for attenuation, and integrated. Two nuclear medicine specialists who were unaware of the patient clinical information evaluated the 18F-FDG PET/CT scans. For semiquantitative analysis, a three-dimensional volume of interest (VOI) was drawn for each lesion as well as for spheroidal normal liver tissue (D=3 cm, as non-tumor tissue) using Ture-D software in a Siemens Biograph workstation.
TSUV =Tumor SUV
LSUV=Liver SUV
ΔTSUVmax= TSUVmax(PET/CT1) - TSUVmax(PET/CT2)
ΔTSUVmax%=[TSUVmax(PET/CT1) - TSUVmax(PET/CT2)]/ TSUVmax(PET/CT1)
ΔTSUVmean= TSUVmean(PET/CT1) - TSUVmean(PET/CT2)
ΔTSUVmean%=[TSUVmean(PET/CT1) - TSUVmean(PET/CT2)]/ TSUVmean(PET/CT1)
Δ(TSUVmax/LSUVmean)=ΔSUVratio=TSUVmax/LSUVmean(PET/CT1)-TSUVmax/LSUVmean(PET/CT2)
Δ(TSUVmax/LSUVmean)%=ΔSUVratio%=[TSUVmax/LSUVmean(PET/CT1) -TSUVmax/
LSUVmean(PET/CT2)]/ TSUVmax/LSUVmean(PET/CT1)
Statistical Analysis
All quantitative data are presented as the median values with ranges, unless otherwise noted. The area under the receiver operating characteristics (ROC) curves was used to compare the prognostic value of the SUVs and generate a cutoff point. A Mann-Whitney U test was used to compare continuous variables, and a Chi-squared test was used to compare categorical variables, between the PET/CT responders and non-responders. The Kaplan-Meier test was used to generate the survival curves, and the survival difference between the groups was estimated by the log-rank test. Univariate and multivariate Cox regression analyses were used to test the OS prognostic factors. SPSS ver. 16 (SPSS Inc. Chicago, IL, USA) was used to perform the analyses. Statistical significance was defined by a p value < 0.05 or a 95% confidence interval that did not include 1.
Results
Patient characteristics
The patient and treatment characteristics are outlined in Table 1. A total of 27 patients were diagnosed with intermediate-stage HCC according to the BCLC staging system. The follow-up ended on July 2nd, 2013, and the median follow-up time was 12.6 months (range, 1.8-25.2 months). The median age was 54 years (range of 28-72 years). The study included 23 males and 4 females, and the most common etiology was hepatitis B or C virus infection (85.2%). All patients had an ECOG performance status of 0. Twenty-six (96.3%) patients had Child-Pugh class A and 15 (55.6%) had cirrhosis. The median tumor size was 9.2 cm (range, 5.2-16.0cm). Twenty-six (96.3%) patients had 1-2 nodules and 1 (3.7%) patient had 4 nodules. The median number of TACE sessions was two (range, 1~6). The baseline AFP was <200 ng/ml in 13 patients (48.1%) and ≥200 ng/ml in 14 patients (51.9%).
SUV variation cutoff point
The areas under the ROC curve of the ΔTSUVmax, ΔTSUVmax%, ΔTSUVmean, ΔTSUVmean%, Δ(TSUVmax/LSUVmean) and Δ(TSUVmax/LSUVmean)% were 0.66, 0.72, 0.69, 0.54, 0.62 and 0.67, respectively. Thus, the ΔTSUVmax% had the most discriminative prognostic value, and the cutoff of the PET/CT response was 0.1 with a sensitivity of 100% and a specificity of 95.2%. The patients with ≥0.1 for the ΔTSUVmax% were considered PET/CT responders, and the patients with <0.1 for the ΔTSUVmax% were considered PET/CT non-responders. Example images for three patients according to the ΔTSUVmax% are shown in Figures 3, 4 and 5.
Comparison of the baseline clinical characteristics between the PET/CT responders and non-responders
In this study, 12(44.4%) and 15(55.6%) patients were PET/CT responders and non-responders, respectively. None of the baseline clinical characteristics, including their age, sex, etiology, Child-Pugh class, cirrhosis, size and number of tumors, number of TACE sessions and laboratory tests, were significantly different between the two groups (Table 1).
The relationship between the PET/CT response and contrast-enhanced CT evaluation
For the mRECIST criteria evaluation, there were 18 (66.7%) contrast-enhanced CT responders, and 9 (33.3%) contrast-enhanced CT non-responders. We compared the baseline ΔTSUVmax, ΔTSUVmax%, ΔTSUVmean, ΔTSUVmean%, Δ(TSUVmax/LSUVmean) and Δ(TSUVmax/LSUVmean)% between the mRECIST responders and non-responders. Finally, there was a statistically significant difference between the two groups for the ΔTSUVmax% (0.46 vs. -0.61, p=0.027). The PET/CT response was strongly related to the mRECIST criteria response (Table 2).
Baseline clinical characteristics
| Variable | All Patients (n=27) | PET-CT Response (n=12) | PET-CT Non-Response (n=15) | P value |
|---|---|---|---|---|
| Age (y) | ||||
| Median (Range) | 54 (28-72) | 53.5 (34-72) | 55 (28-71) | 0.751 |
| Sex | ||||
| Male/Female - No. (%) | 23 (85.2%)/ 4 (14.8%) | 10 (83.3%)/ 2 (16.7%) | 13 (86.7%)/ 2 (13.3%) | 1.000 |
| Etiology | ||||
| HBV/HCV+Other - No. (%) | 23 (85.2%)/ 4 (14.8%) | 10 (83.3%)/ 2 (16.7%) | 13 (86.7%)/ 2 (13.3%) | 1.000 |
| Child-Pugh class | ||||
| A/B - No. (%) | 26 (96.3%)/ 1 (3.7%) | 12 (100%)/ 0 (0%) | 14 (93.3%)/ 1 (6.7%) | 1.000 |
| ECOG | ||||
| 0/1 - No. (%) | 27 (100%)/ 0 (0%) | 12 (100%)/ 0 (0%) | 15 (100%)/ 0 (0%) | / |
| BCLC stage | ||||
| B/C - No. (%) | 27 (100%)/ 0 (0%) | 12 (100%)/ 0 (0%) | 15 (100%)/ 0 (0%) | / |
| Cirrhosis | ||||
| Yes/Unknown - No. (%) | 15 (55.6%)/ 12 (44.4%) | 7 (58.3%)/ 5 (41.7%) | 8 (53.3%)/ 7 (46.7%) | 0.795 |
| Disease burden | ||||
| PVTT | ||||
| Yes/No - No. (%) | 0 (0%)/ 27 (100%) | 0 (0%)/ 12 (100%) | 0 (0%)/ 15 (100%) | / |
| Extrahepatic spread | ||||
| Yes/No - No. (%) | 0 (0%)/ 27 (100%) | 0 (0%)/ 12 (100%) | 0 (0%)/ 15 (100%) | / |
| Baseline tumor size (cm) | ||||
| Median (Range) | 9.2 (5.2-16) | 7.65 (5.2-15.5) | 9.8 (5.8-16) | 0.071 |
| No. of HCC nodules | ||||
| 1-2/≥3- No. (%) | 26 (96.3%)/ 1 (3.7%) | 12 (100%)/ 0 (0%) | 14 (93.3%)/ 1 (6.7%) | 1.000 |
| Baseline AFP (ng/ml) | ||||
| <200/≥ 200 - No. (%) | 13 (48.1%)/ 14 (51.9%) | 7 (58.3%)/ 5 (41.7%) | 6 (40%)/ 9 (40%) | 0.343 |
| Liver biopsy | ||||
| Yes/No - No. (%) | 15 (55.6%)/ 12 (44.4%) | 7 (58.3%)/ 5 (41.7%) | 8 (53.3%)/ 7 (46.7%) | 0.795 |
| Ascites | ||||
| Yes/No - No. (%) | 2 (7.4%)/ 25 (92.6%) | 0 (0%)/ 12 (100%) | 2 (13.3%)/ 13 (86.7%) | 0.487 |
| No. of TACE | ||||
| Median (Range) | 2 (1-6) | 1 (1-6) | 2 (1-5) | 0.337 |
| Baseline laboratory values | ||||
| White blood cell, *10E9/L | ||||
| Median (Range) | 5 (3.07-9.35) | 4.15 (3.07-8.14) | 5.38 (3.19-9.35) | 0.137 |
| Hemoglobin, g/L | ||||
| Median (Range) | 134 (97-176) | 133.5 (121-151) | 138 (97-176) | 0.420 |
| Platelets, *10E9/L | ||||
| Median (Range) | 154 (60-263) | 122 (60-225) | 172 (63-263) | 0.113 |
| Alanine aminotransferase, IU/L | ||||
| Median (Range) | 43 (12-114) | 35.5 (12-82) | 47 (23-114) | 0.092 |
| Aspartate aminotransferase, IU/L | ||||
| Median (Range) | 45 (13-166) | 36.5 (13-109) | 62 (21-166) | 0.088 |
| Albumin, g/L | ||||
| Median (Range) | 38.8 (31-48) | 38.6 (33.2-48) | 38.8 (31-47.4) | 0.826 |
| Total bilirubin, umol/L | ||||
| Median (Range) | 14.2 (5.2-28.3) | 14 (5.2-22.4) | 14.2 (7.2-28.3) | 0.770 |
| Serum creatinine, umol/L | ||||
| Median (Range) | 74 (53-114) | 72.5 (61-114) | 74 (53-90) | 0.283 |
| International normalized ratio | ||||
| Median (Range) | 1.12 (0.92-1.43) | 1.07 (0.92-1.25) | 1.12 (1.05-1.43) | 0.070 |
Abbreviations: PET-CT, positron emission tomography-computed tomography; HBV, hepatitis B virus; HCV, hepatitis C virus; ECOG, Eastern Cooperative Oncology Group; BCLC, Barcelona Clinic Liver Cancer; PVTT, portal vein tumor thrombosis; HCC, hepatocellular carcinoma; AFP, alpha-fetoprotein;TACE, transarterial chemoembolization.
Correlation between PET/CT assessment and contrast-enhanced CT evaluation
| PET-CT evaluation | mRECIST | P value | |
|---|---|---|---|
| Response (CR+PR) (n=18) | Non-Response (SD+PD) (n=9) | ||
| TSUVmax(Baseline) | 4.9 | 7.36 | 0.476 |
| TSUVmax/LSUVmean(Baseline) | 2.98 | 3.85 | 0.356 |
| ΔTSUVmax | 0.48 | -0.53 | 0.06 |
| ΔTSUVmax% | 0.46 | -0.61 | 0.027 |
| ΔTSUVmean | 0.16 | -0.11 | 0.054 |
| ΔTSUVmean% | 0.095 | -0.08 | 0.06 |
| Δ(TSUVmax/LSUVmean) | 0.29 | -0.46 | 0.72 |
| Δ(TSUVmax/LSUVmean)% | 0.08 | -0.12 | 0.105 |
Abbreviations: PET-CT, positron emission tomography-computed tomography; mRECIST, Modified Response Evaluation Criteria in Solid Tumor; CR, complete response; PR, partial response; SD, stable disease; PD, progressive disease; SUV, standard uptake value.
The relationship between the PET/CT response and survival
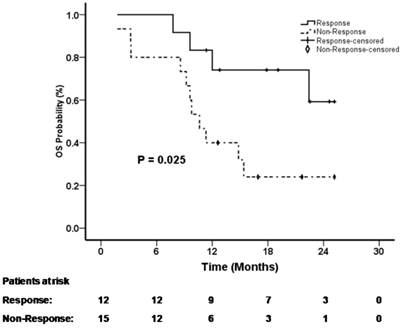
The median OS for all patients was 15.4 months (95%CI, 3.3-27.5 months). The cumulative OS rates in the PET/CT responders at 6, 12, 18 and 24 months were 100%, 83.3%, 74.1% and 59.3%, respectively. The cumulative OS rates in the PET/CT non-responders were 80%, 40%, 24% and 24%, respectively. The OS was significantly better for the PET/CT responders than for PET/CT non-responders (p=0.025) (Figure 1).
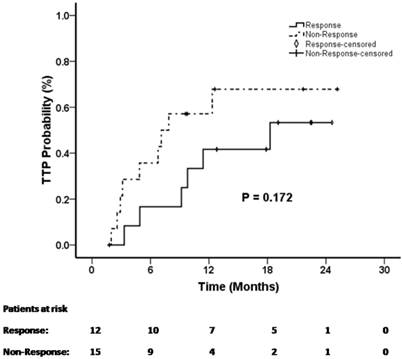
The median TTP for all patients was 11.4 months (95%CI, 6.7-16.1 months). The median TTP was 18.3 months in the PET/CT responders and 7.1 months in the PET/CT non-responders. The median TTP for the PET/CT responders trended towards, but was no significantly higher than for the PET/CT non-responders (p=0.172) (Figure 2).
Univariate analysis demonstrated that the liver biopsy and PET/CT response were the prognostic factors for the OS (Table 3). Multivariate analysis further confirmed that the liver biopsy (HR=3.65, 95%CI, 1.22-10.91; p=0.021) and PET/CT response (HR=4.05, 95%CI, 1.21-13.60; p=0.024) were independent prognostic factors for the OS (Table 3).
The median OS for all patients was 15.4 months (95%CI, 3.3-27.5 months). The OS was significantly better in the PET/CT response group than in the PET/CT non-response group (p=0.025).
The median TTP for all patients was 11.4 months (95%CI, 6.7-16.1 months). The median TTP for the PET/CT responders was higher than for the PET/CT non-responders; however, this difference was not statistically significant (p=0.172).
Independent predictors for overall survival
| Variable | Univariate analysis | Multivariate analysis | ||||
|---|---|---|---|---|---|---|
| HR | 95%CI | P value | HR | 95%CI | P value | |
| Age (y) | 0.97 | 0.932-1.010 | 0.14 | / | / | / |
| Sex | ||||||
| Male vs. Female | 0.685 | 0.190-2.468 | 0.563 | / | / | / |
| Etiology | ||||||
| HBV vs. HCV+Other | 3.151 | 0.414-24.001 | 0.268 | / | / | / |
| Child-Pugh class | ||||||
| B vs. A | 0.045 | 0.000-1.399 | 0.558 | / | / | / |
| Cirrhosis | ||||||
| Unknown vs. Yes | 1.264 | 0.448-3.566 | 0.658 | / | / | / |
| Baseline tumor size (cm) | 1.05 | 0.899-1.225 | 0.54 | / | / | / |
| No. of HCC nodules | ||||||
| ≥3 vs. 1-2 | 1.565 | 0.203-12.094 | 0.668 | / | / | / |
| Baseline AFP (ng/ml) | ||||||
| ≥ 200 vs. <200 | 2.256 | 0.767-6.631 | 0.139 | / | / | / |
| Liver biopsy | ||||||
| No vs. Yes | 3.24 | 1.104-9.509 | 0.032 | 3.65 | 1.221-10.914 | 0.021 |
| Ascites | ||||||
| Yes vs. No | 0.687 | 0.089-5.275 | 0.718 | / | / | / |
| No. of TACE | 0.857 | 0.560-1.310 | 0.476 | / | / | / |
| PET-CT | ||||||
| Non-response vs. Response | 3.529 | 1.094-11.385 | 0.035 | 4.051 | 1.207-13.600 | 0.024 |
Abbreviations: HBV, hepatitis B virus; HCV, hepatitis C virus; ECOG, Eastern Cooperative Oncology Group; BCLC, Barcelona Clinic Liver Cancer; PVTT, portal vein tumor thrombosis; HCC, hepatocellular carcinoma; AFP, alpha-fetoprotein;TACE, transarterial chemoembolization; PET-CT, positron emission tomography-computed tomography.
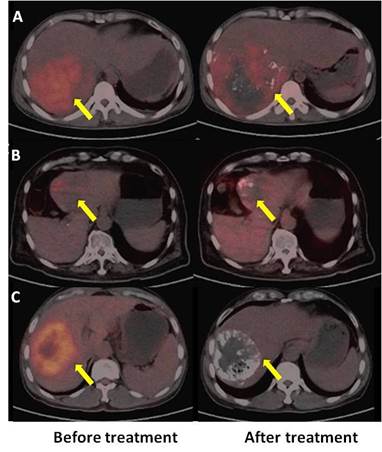
A: PET, B: CT, C: PET/CT fused axial imaging, and D: enhanced CT. Baseline and follow-up images after TACE in a 37-year-old male patient with HCC (once TACE, OS 3.23 m, PET no response, mRECIST SD). The time elapsed after TACE was 31 d for enhanced CT and 35 d for the PET/CT scan, respectively. There was high tumor uptake in the first PET scan (left) and higher local lesion uptake in the second scan (right), indicating a poor prognosis after TACE. Early PET after therapy provided a more accurate evaluation than enhanced CT.
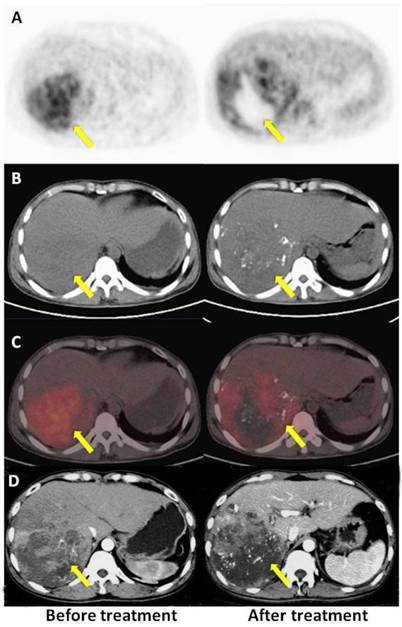
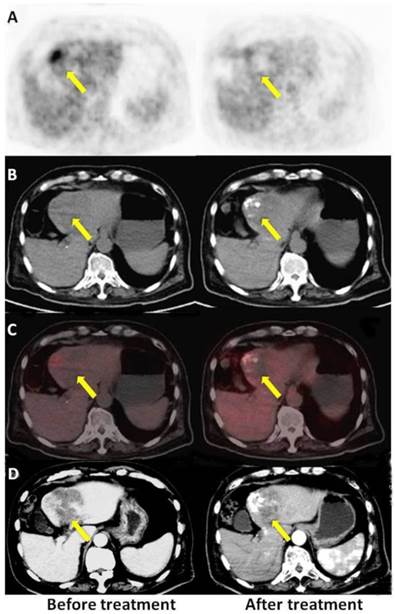
A: PET, B: CT, C: PET/CT fused axial images, and D: enhanced CT. A 70-year-old male with HCC (once TACE, OS 9.77 m, mRECIST PR, PET no response). The time elapsed after TACE was 30 d for enhanced CT and 34 d for the PET/CT scan, respectively. There was high tumor uptake in the first PET scan (left) and relatively low uptake in the second scan (right) after therapy, but the patient belonged to the PET non-response group, indicating a poor prognosis.
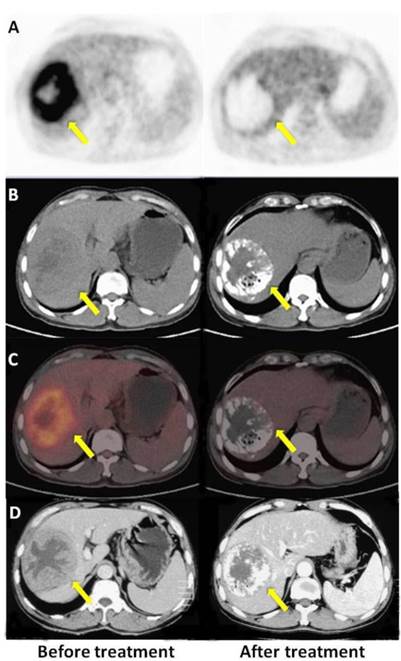
A: PET, B: CT, C: PET/CT fused axial images, and D: enhanced CT. A 60-year-old male with HCC (once TACE, OS 24.6 m, mRECIST CR, PET response). The time elapsed after TACE was 31 d for enhanced CT and 32 d for the PET/CT scan, respectively. Compared with high tumor uptake in the first PET scan (left), there was no 18F-FDG uptake in the tumor or surrounding tissue in the second scan (right). Both PET/CT and enhanced CT indicated a good response to treatment.
Discussion
We evaluated the efficacy and prognosis of 18F-FDG PET/CT in 27 HCC patients during TACE therapy. The ΔTSUVmax% in the first month after TACE has potential prognostic value for HCC patients. To the best of our knowledge, this is the first study focusing on the prognostic value of the 18F-FDG PET/CT parameter changes in HCC patients treated with TACE.
The semi-quantitative parameters, such as the SUV, were affected by the degree of tumor differentiation, whole tumor necrosis size and degree of underlying cirrhosis in the baseline scan. We found that the SUV change was objectively better at predicting patient survival after TACE. Furthermore, it is reasonable to evaluate these differences by comparing the target versus background range of semiquantitative SUVs. Meanwhile, patients with an adjusted ΔTSUVmax%≥0.1 had a better OS rate than the patients with a ΔTSUVmax%<0.1. With Cox regression analysis, we also found that the ΔTSUVmax% was an independent prognostic factor for the OS. Moreover, the ΔTSUVmax% was strongly related to the mRECIST criteria assessment.
Although factors such as the ECOG PS, AFP concentration, and portal vein thrombosis were significantly related to survival in other studies, the SUVs from 18F-FDG PET have several advantages over the other potential biological or imaging markers. The SUV reflects the tumor cell biology regardless of the treatment status [15]. The SUV ratio correlates with the tumor volume doubling time and cumulative survival rate for primary HCC; a high SUV ratio signifies more malignant tumors and, thus, a worse prognosis [20]. Many previous studies have focused on semi-quantitative parameters such as the simple TSUVmax and have related them to the survival time after several treatments, such as traditional chemotherapy, radiotherapy, resection, TACE and Sorafenib [9,15-18]. Lee et al. found that the tumor SUVmax is a good prognostic factor and Song et al. confirmed that the TSUVmax/LSUVmean (SUV ratio) is the better prognostic factor [17,18]. Thus the degree of FDG uptake (SUV ratio) in HCC should be a useful prognostic marker.
The median OS was 15.4 months for the entire cohort (Figure 1). Unfortunately, TACE of large HCC is predisposed to unsatisfactory long-term outcomes. One potential reason for this may be the increase in the plasma vascular endothelial growth factor (VEGF) levels after TACE [21,22]. Disturbances in the tumor microenvironment following TACE lead to increased hypoxia and up-regulation in hypoxia inducible factor-1a, VEGF and platelet-derived growth factor receptor (PDGFR), resulting in tumor angiogenesis [21,22]. These effects may also explain the enhanced 18F-FDG uptake around the tumor after TACE in patients with shorter survival times (Figure 3) [23,24]. Therefore, 18F-FDG PET/CT still provides a useful tool for the early prediction of a patient' prognosis after TACE.
18F-FDG PET/CT is a well-established functional imaging technique for diagnostic oncological imaging that provides information about the glucose metabolism of lesions. In contrast with contrast-enhanced ultrasonography (CEUS), PET/CT is not operator dependent. As a whole body surveillance imaging technique, PET/CT, unlike for CT or MRI, does not require dedicated software for performing calculations and can be used to evaluate both primary and metastatic lesions in a single study. In this study, 100% of the lesions were visible by PET/CT imaging, and eight patients were excluded after baseline scans. The baseline PET/CT scan can predict the patient' prognosis, decreasing unnecessary financial costs and patient suffering. An interim PET scan after TACE was also performed to monitor the early treatment response, which provided more useful therapy evaluation than the baseline scan (Figure 1).
There are several limitations to this study. First, the small sample size may result in statistical bias and inaccurate conclusions, which may explain the lack of a relationship between the AFP level and SUV in our study [17]. Next, the patients underwent different treatment regimens, according to their needs after the second PET/CT, which may have influenced their outcomes. Although we found a significant relationship between the degree and ratio change of 18F-FDG uptake with the prognosis, the 18F-FDG PET SUV, unlike with biomarkers, is not an independent indicator of progression in HCC patients. Lastly, although FDG PET/CT has a low sensitivity for HCC, PET/CT has an important role in predicting the prognosis for HCC patients [18].
Conclusion
18F-FDG PET/CT has diagnostic value in detecting viable HCC patients. We found that the ΔTSUVmax% from early interim PET/CT after TACE is helpful in predicting the HCC patient prognosis, which may help determine the viability of HCCs in patients with high baseline SUVs on follow-up. Therefore, 18F-FDG PET/CT may provide valuable information that can be used in the treatment response evaluation and clinical decision making process. Furthermore, a well-designed, larger cohort of patients is still needed to validate the results of this study.
Acknowledgements
The authors would like to thank Jing Niu and Shuna Zhang for their efforts in preserving all imaging data and follow-up surveillance in this study. This work was supported by the Key Program of the National Natural Science Foundation of China (Grant No. 81230033), The Major State Basic Research Development Program (Grant No. 2011CB707704), The Major Instrument of National Natural Science Foundation Research Project (Grant No. 81227901 and 81172145), the Major Program of National Natural Science Foundation of China (Grant No. 81090270), the General Program of National Natural Science Foundation of China(Grant No. 81371594) and the International Cooperation Program of Xijing Hospital (Grant No. XJZT13G02).
Competing Interests
The authors have declared that no competing interest exists.
References
1. Trevisani F, De Notariis S, Rossi C, Bernardi M. Randomized control trials on chemoembolization for hepatocellular carcinoma: is there room for new studies? J Clin Gastroenterol. 2001;32:383-9
2. Llovet JM, Bruix J. Systematic review of randomized trials for unresectable hepatocellular carcinoma: Chemoembolization improves survival. Hepatology. 2003;37:429-42
3. Bruix J, Sala M, Llovet JM. Chemoembolization for hepatocellular carcinoma. Gastroenterology. 2004;127:S179-88
4. Lo CM, Ngan H, Tso WK, Liu CL, Lam CM, Poon RT, Fan ST, Wong J. Randomized controlled trial of transarterial lipiodol chemoembolization for unresectable hepatocellular carcinoma. Hepatology. 2002;35:1164-71
5. Llovet JM, Real MI, Montana X, Planas R, Coll S, Aponte J, Ayuso C, Sala M, Muchart J, Sola R, Rodes J, Bruix J. Arterial embolisation or chemoembolisation versus symptomatic treatment in patients with unresectable hepatocellular carcinoma: a randomised controlled trial. Lancet. 2002;359:1734-9
6. EASL-EORTC clinical practice guidelines. management of hepatocellular carcinoma. J Hepatol. 2012;56:908-43
7. Bruix J, Sherman M. Management of hepatocellular carcinoma: an update. Hepatology. 2011;53:1020-2
8. Shim JH, Lee HC, Kim SO, Shin YM, Kim KM, Lim YS, Suh DJ. Which response criteria best help predict survival of patients with hepatocellular carcinoma following chemoembolization? A validation study of old and new models. Radiology. 2012;262:708-18
9. Seo S, Hatano E, Higashi T, Hara T, Tada M, Tamaki N, Iwaisako K, Ikai I, Uemoto S. Fluorine-18 fluorodeoxyglucose positron emission tomography predicts tumor differentiation, P-glycoprotein expression, and outcome after resection in hepatocellular carcinoma. Clin Cancer Res. 2007;13:427-33
10. Shiomi S, Nishiguchi S, Ishizu H, Iwata Y, Sasaki N, Tamori A, Habu D, Takeda T, Kubo S, Ochi H. Usefulness of positron emission tomography with fluorine-18-fluorodeoxyglucose for predicting outcome in patients with hepatocellular carcinoma. Am J Gastroenterol. 2001;96:1877-80
11. Higashi T, Hatano E, Ikai I, Nishii R, Nakamoto Y, Ishizu K, Suga T, Kawashima H, Togashi K, Seo S, Kitamura K, Takada Y, Uemoto S. FDG PET as a prognostic predictor in the early post-therapeutic evaluation for unresectable hepatocellular carcinoma. Eur J Nucl Med Mol Imaging. 2010;37:468-82
12. Lee JW, Paeng JC, Kang KW, Kwon HW, Suh KS, Chung JK, Lee MC, Lee DS. Prediction of tumor recurrence by 18F-FDG PET in liver transplantation for hepatocellular carcinoma. J Nucl Med. 2009;50:682-7
13. Ahn SG, Kim SH, Jeon TJ, Cho HJ, Choi SB, Yun MJ, Lee JD, Kim KS. The role of preoperative [18F]fluorodeoxyglucose positron emission tomography in predicting early recurrence after curative resection of hepatocellular carcinomas. J Gastrointest Surg. 2011;15:2044-52
14. Lee JD, Yun M, Lee JM, Choi Y, Choi YH, Kim JS, Kim SJ, Kim KS, Yang WI, Park YN, Han KH, Lee WJ, Yoo N, Lim SM, Park JH. Analysis of gene expression profiles of hepatocellular carcinomas with regard to 18F-fluorodeoxyglucose uptake pattern on positron emission tomography. Eur J Nucl Med Mol Imaging. 2004;31:1621-30
15. Shin DY, Han SW, Oh DY, Im SA, Kim TY, Bang YJ. Prognostic implication of (18)F FDG-PET in patients with extrahepatic metastatic hepatocellular carcinoma undergoing systemic treatment, a retrospective cohort study. Cancer Chemother Pharmacol. 2011;68:165-75
16. Kim JW, Seong J, Yun M, Lee IJ, Yoon HI, Cho HJ, Han KH. Usefulness of positron emission tomography with fluorine-18-fluorodeoxyglucose in predicting treatment response in unresectable hepatocellular carcinoma patients treated with external beam radiotherapy. Int J Radiat Oncol Biol Phys. 2012;82:1172-8
17. Song MJ, Bae SH, Lee SW, Song do S, Kim HY, Yoo Ie R, Choi JI, Lee YJ, Chun HJ, Lee HG, Choi JY, Yoon SK. 18F-fluorodeoxyglucose PET/CT predicts tumour progression after transarterial chemoembolization in hepatocellular carcinoma. Eur J Nucl Med Mol Imaging. 2013;40:865-73
18. Lee JH, Park JY, Kim do Y, Ahn SH, Han KH, Seo HJ, Lee JD, Choi HJ. Prognostic value of 18F-FDG PET for hepatocellular carcinoma patients treated with sorafenib. Liver Int. 2011;31:1144-9
19. Lei Liu, Weijuan Wang, Hui Chen, Yan Zhao, Wei Bai, Zhanxin Yin, Chuangye He, Jia Jia, Man Yang, Jielai Xia, Daiming Fan, Guohong Han. EASL- and mRECIST-evaluated responses to combination therapy predict survival in patients with hepatocellular carcinoma. Clin Cancer Res. 2014 accepted
20. Zhu AX, Sahani DV, Duda DG, di Tomaso E, Ancukiewicz M, Catalano OA, Sindhwani V, Blaszkowsky LS, Yoon SS, Lahdenranta J, Bhargava P, Meyerhardt J, Clark JW, Kwak EL, Hezel AF, Miksad R, Abrams TA, Enzinger PC, Fuchs CS, Ryan DP, Jain RK. Efficacy, safety, and potential biomarkers of sunitinib monotherapy in advanced hepatocellular carcinoma: a phase II study. J Clin Oncol. 2009;27:3027-35
21. Li X, Feng GS, Zheng CS, Zhuo CK, Liu X. Expression of plasma vascular endothelial growth factor in patients with hepatocellular carcinoma and effect of transcatheter arterial chemoembolization therapy on plasma vascular endothelial growth factor level. World J Gastroenterol. 2004;10:2878-82
22. Wang B, Xu H, Gao ZQ, Ning HF, Sun YQ, Cao GW. Increased expression of vascular endothelial growth factor in hepatocellular carcinoma after transcatheter arterial chemoembolization. Acta Radiol. 2008;49:523-9
23. Tseng CS, Lo HW, Chen PH, Chuang WL, Juan CC, Ker CG. Clinical significance of plasma D-dimer levels and serum VEGF levels in patients with hepatocellular carcinoma. Hepatogastroenterology. 2004;51:1454-8
24. Kaseb AO, Hassan MM, Lin E, Xiao L, Kumar V, Pathak P, Lozano R, Rashid A, Abbruzzese JL, Morris JS. V-CLIP: Integrating plasma vascular endothelial growth factor into a new scoring system to stratify patients with advanced hepatocellular carcinoma for clinical trials. Cancer. 2011;117:2478-88
Author contact
Corresponding author: Prof. G. H. Han, Department of Liver Disease and Digestive Interventional Radiology, Xijing Hospital of Digestive Diseases, Xijing Hospital, Fourth Military Medical University, 15 West Changle Road, Xi'an 710032, China. E-mail: hanghedu.cn or Prof. J Wang, Department of Nuclear Medicine, Xijing Hospital, Fourth Military Medical University, 15 West Changle Road, Xi'an 710032, Shaanxi, China. E-mail: wangjingedu.cn.
 Global reach, higher impact
Global reach, higher impact