13.3
Impact Factor
Theranostics 2019; 9(7):2084-2099. doi:10.7150/thno.29463 This issue Cite
Research Paper
HOXB13 networking with ABCG1/EZH2/Slug mediates metastasis and confers resistance to cisplatin in lung adenocarcinoma patients
1. Key Laboratory of Carcinogenesis and Translational Research (Ministry of Education), and State Key Laboratory of Natural and Biomimetic Drugs, Peking University Health Science Center, Beijing 100191, China;
2. Institute of Cardiovascular Research, Peking University Health Science Center, Beijing 100191, China;
3. Medical Isotopes Research Center and Department of Radiation Medicine, School of Basic Medical Sciences, Peking University Health Science Center, Beijing 100191, China;
4. Department of Internal Medicine, Cancer Hospital Chinese Academy of Medical Sciences, Beijing 100021, China;
5. School of Pharmaceutical Sciences, Peking University Health Science Center, Beijing 100191, China;
6. School of Medicine, Tsinghua University.
Abstract
Rationale: Distant metastasis and chemoresistance are the major causes of short survival after initial chemotherapy in lung adenocarcinoma patients. However, the underlying mechanisms remain elusive. Our pilot study identified high expression of the homeodomain transcription factor HOXB13 in chemoresistant lung adenocarcinomas. We aimed to investigate the role of HOXB13 in mediating lung adenocarcinoma chemoresistance.
Methods: Immunohistochemistry assays were employed to assess HOXB13 protein levels in 148 non-small cell lung cancer patients. The role of HOXB13 in lung adenocarcinoma progression and resistance to cisplatin therapy was analyzed in cells, xenografted mice, and patient-derived xenografts. Needle biopsies from 15 lung adenocarcinoma patients who were resistant to cisplatin and paclitaxel therapies were analyzed for HOXB13 and EZH2 protein levels using immunohistochemistry.
Results: High expression of HOXB13 observed in 17.8% of the lung adenocarcinoma patients in this study promoted cancer progression and predicted poor prognosis. HOXB13 upregulated an array of metastasis- and drug-resistance-related genes, including ABCG1, EZH2, and Slug, by directly binding to their promoters. Cisplatin induced HOXB13 expression in lung adenocarcinoma cells, and patient-derived xenografts and depletion of ABCG1 enhanced the sensitivity of lung adenocarcinoma cells to cisplatin therapy. Our results suggest that determining the combined expression of HOXB13 and its target genes can predict patient outcomes.
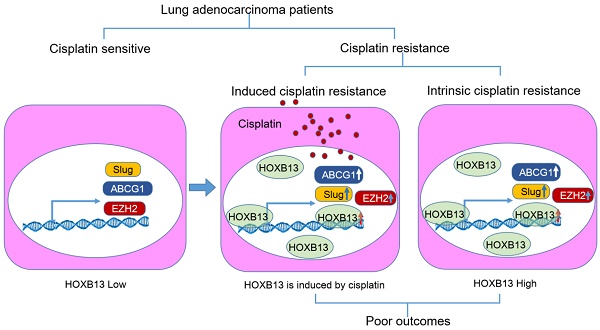
Conclusions: A cisplatin-HOXB13-ABCG1/EZH2/Slug network may account for a novel mechanism underlying cisplatin resistance and metastasis after chemotherapy. Determining the levels of HOXB13 and its target genes from needle biopsy specimens may help predict the sensitivity of lung adenocarcinoma patients to platinum-based chemotherapy and patient outcomes.
Keywords: HOXB13, metastasis, cisplatin resistance, prognosis, lung adenocarcinoma
 Global reach, higher impact
Global reach, higher impact