Impact Factor
Theranostics 2017; 7(4):945-951. doi:10.7150/thno.19102 This issue Cite
Research Paper
Association of γH2AX at Diagnosis with Chemotherapy Outcome in Patients with Breast Cancer
1. National Clinical Target Validation Laboratory, Division of Cancer Treatment and Diagnosis, National Cancer Institute, National Institutes of Health, Bethesda, Maryland, United States;
2. Division of Biomedical Statistics and Informatics, Department of Health Sciences Research, Mayo Clinic, Rochester, Minnesota, United States.
Abstract
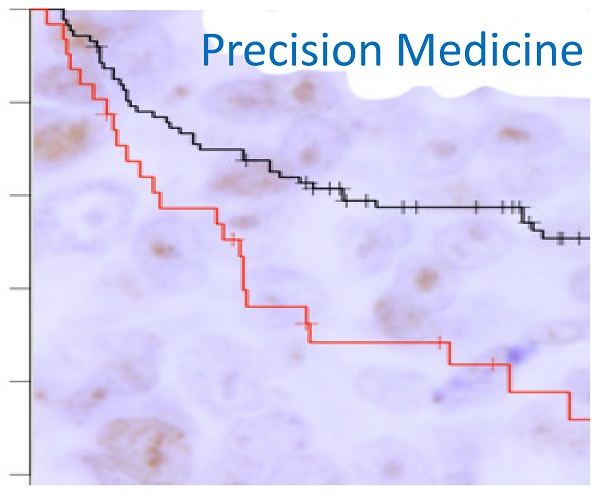
γH2AX plays a role in DNA damage response signaling and facilitates the repair of DNA double strand breaks. However, it remains unknown whether constitutive tumor γH2AX expression is associated with treatment outcome in patients. γH2AX status was detected in primary tumors from 24% of 826 patients with stage I, II and III breast cancer by immunohistochemistry; overall survival was analyzed by Kaplan-Meier method. At median follow-up of 176 months (range 13 - 282 months), we found substantial survival heterogeneity in γH2AX-positive patients (P=0.002) among uniform treatment groups including radiation or endocrine therapy alone and no-treatment, as well as chemotherapy alone (being worst), in contrast to γH2AX-negative patients (P=0.2). In the chemotherapy group (n=118), median survival was 63 months (95% confidence interval [CI], 29 - 83) in patients with γH2AX-positive tumors compared with 170 months (95% CI 94 - 235) in those with γH2AX-negative tumors (P=0.0017). γH2AX remained a poor prognosis factor in the group by multivariable analysis (adjusted hazard ratio 2.12, P=0.009). Our data demonstrate that constitutive γH2AX positivity is significantly associated with survival heterogeneity in patients among uniform treatment groups, and its expression at diagnosis independently predicts poor chemotherapy outcome in breast cancer.
Keywords: breast cancer, chemotherapy, γH2AX expression, overall survival, standard therapy.
 Global reach, higher impact
Global reach, higher impact